The Precuneus and Recovery From a Minimally Conscious State
 You've probably heard about the case of Terry Wallis, a 42 year old man in Arkansas who spent 19 years in a "minimally conscious state" following severe traumatic brain injury. Then one day he saw his mother walk into the room and (after not speaking all those years) said "Mom."
You've probably heard about the case of Terry Wallis, a 42 year old man in Arkansas who spent 19 years in a "minimally conscious state" following severe traumatic brain injury. Then one day he saw his mother walk into the room and (after not speaking all those years) said "Mom."The Aspen workgroup defined the minimally conscious state (MCS) as a condition of severely altered consciousness in which the person demonstrates minimal but definite behavioral evidence of self or environmental awareness (Giacino et al, 1997).A number of bloggers have commented on how his case is different from that of Terry Schiavo, who was in a persistent vegetative state (not a MCS).
What I'll focus on here is the work of researchers at Cornell, who followed Mr. Wallis using diffusion tensor imaging (DTI) and PET scanning over an 18 month period.
Using a novel technique, they saw evidence of new growth in the midline cerebellum, an area involved in motor control, as Mr. Wallis gained strength and range in his limbs. Another area of new growth, located along the back of the brain, is believed by some experts to be a central switching center for conscious awareness.The "central switching center for conscious awareness" is the precuneus, interestingly enough.
The daily exercises, the interactions with his parents, his regular dose of antidepressant medication: any or all of these might have spurred brain cells to grow more connections, the researchers said.
"The big missed opportunity is that we didn't know this guy would spontaneously emerge, and we didn't get to monitor him before then" to find out what preceded it, Dr. Schiff said.
Henning U. Voss, Aziz M. Uluç, Jonathan P. Dyke, Richard Watts, Erik J. Kobylarz, Bruce D. McCandliss, Linda A. Heier, Bradley J. Beattie, Klaus A. Hamacher, Shankar Vallabhajosula, Stanley J. Goldsmith, Douglas Ballon, Joseph T. Giacino and Nicholas D. Schiff. (2006). Possible axonal regrowth in late recovery from the minimally conscious state. J. Clin. Invest. 116: 2005-2011. OPEN ACCESS ARTICLE!In a commentary on the article, Laureys, Boly, and Maquet note the importance of the precuneus in conscious awareness:
We used diffusion tensor imaging (DTI) to study 2 patients with traumatic brain injury. The first patient recovered reliable expressive language after 19 years in a minimally conscious state (MCS); the second had remained in MCS for 6 years. Comparison of white matter integrity in the patients and 20 normal subjects using histograms of apparent diffusion constants and diffusion anisotropy identified widespread altered diffusivity and decreased anisotropy in the damaged white matter. These findings remained unchanged over an 18-month interval between 2 studies in the first patient. In addition, in this patient, we identified large, bilateral regions of posterior white matter with significantly increased anisotropy that reduced over 18 months. In contrast, notable increases in anisotropy within the midline cerebellar white matter in the second study correlated with marked clinical improvements in motor functions. This finding was further correlated with an increase in resting metabolism measured by PET in this subregion. Aberrant white matter structures were evident in the second patient’s DTI images but were not clinically correlated. We propose that axonal regrowth may underlie these findings and provide a biological mechanism for late recovery. Our results are discussed in the context of recent experimental studies that support this inference.
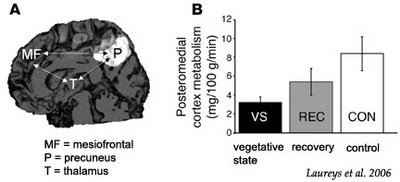
The most remarkable finding in the Voss et al. study (12) was the MRI assessment of transiently increased fractional anisotropy and directionality in the posterior midline cortices (encompassing the cuneus and precuneus), interpreted as increased myelinated fiber densities and novel corticocortical sprouting, paralleling the emergence of the patient from MCS. The same area of the patient’s brain also showed amplified metabolic activity, as measured by PET. This finding stresses the importance of the posterior medial structures in consciousness of self and interaction with the environment (14, 15). Activity in the medial parietal cortex (i.e., precuneus) seems to show it to be the brain region that best differentiates MCS from VS patients (16). Interestingly, this area is among the most active brain regions in conscious waking (15) and is among the least active in altered states of consciousness, such as pharmacological coma (17), sleep (18), dementia (19), Wernicke-Korsakoff syndrome, and postanoxic amnesia (20). It has been suggested that this richly connected multimodal posteromedial associative area is part of the neural network subserving human awareness (21).
 The figure above illustrates Mr. Wallis' brain. On the left is a DTI scan to trace fiber tracts. On the right is a PET scan to measure glucose metabolism. The areas highlighted are on the posterior medial surface of the brain, the parietal-occipital region, which includes the cuneus and precuneus.
The figure above illustrates Mr. Wallis' brain. On the left is a DTI scan to trace fiber tracts. On the right is a PET scan to measure glucose metabolism. The areas highlighted are on the posterior medial surface of the brain, the parietal-occipital region, which includes the cuneus and precuneus.It's really interesting to compare the DTI scan of Mr. Wallis with that of a control subject, as illustrated below. The first thing to note is the degeneration in Patient 1's corpus callosum (the big red crescent in the middle of the control's brain, labeled cc). This structure is a huge white matter tract that connects the two cerebral hemispheres. But what's most novel is the unique white matter tract in Patient 1's parietal-occipital region. Could this presumed axonal growth be the basis of the remarkable improvement in Mr. Wallis' state of awareness?

Steven Laureys, Mélanie Boly and Pierre Maquet (2006). Tracking the recovery of consciousness from coma. J. Clin. Invest. 116:1823-1825. OPEN ACCESS ARTICLE!
Predicting the chances of recovery of consciousness and communication in patients who survive their coma but transit in a vegetative state or minimally conscious state (MCS) remains a major challenge for their medical caregivers. Very few studies have examined the slow neuronal changes underlying functional recovery of consciousness from severe chronic brain damage. A case study in this issue of the JCI reports an extraordinary recovery of functional verbal communication and motor function in a patient who remained in MCS for 19 years (see the related article beginning on page 2005). Diffusion tensor MRI showed increased fractional anisotropy (assumed to reflect myelinated fiber density) in posteromedial cortices, encompassing cuneus and precuneus. These same areas showed increased glucose metabolism as studied by PET scanning, likely reflecting the neuronal regrowth paralleling the patient’s clinical recovery. This case shows that old dogmas need to be oppugned, as recovery with meaningful reduction in disability continued in this case for nearly 2 decades after extremely severe traumatic brain injury.
Terry Wallis at his home in Arkansas.
Mute 19 Years, He Helps Reveal Brain's Mysteries
. . .
He does not feel any physical pain, he told his parents, and he has no real sense of time. He also said recently that he was "proud" to be alive.
"It is good to know all that," said his father, sitting on the porch on Saturday evening.
"It's good to hear him say that, because if he didn't say so, you'd just have no way to know."
Subscribe to Post Comments [Atom]













24 Comments:
Take a look at this:
http://www.yogacara.net/node/7324
It's an exact reproduction of this post. They've done it with at least 5 of my posts as well.
I'm not sure if they're stealing the content, or what to do if they are!
Huh, that's weird. They have an aggregator, too (called "aggregator2"). I suppose they do have a little link at the bottom to the full article.
It would be nice, though, if they more clearly credited their sources...
I have seen here comment of a doctor feeling sarrow that they they did not knew b4 that Terri Wallis will become talking ,He is right but we are here experiencing improvement of my son Jawad Pasha .He is becoming Fully conscious slowly.We here at Pakistan have very less facilities regarding brain injury but perhaps this could be a reason of his improvement.He was a vegetative state but later he improved and than for a period we can call him minimally conscious state but now he can be called fully Conscious or fully aware state.One can search about problems and tragedies we are facing but I am sure now that soon we shall be able to help and gauide many as we are now.
Thanks for your comment, Anwer. I hope your son continues to improve. Best to you and your family.
Thank you
It is less than one month since my last comments,Only due to grace of God Jawad Pasha is further improving. He looks more conscious,we are already sure that he is fully wise,only can not express.I think about thousands like him and also think that what medical science is doing with them ? You looks much aware. Please write again after studying new reports on tnis topic.
writing again about same.Jawad Pasha is futher improved but I am sure that he was fully conscious from day-1 and only his consciousness is discovered.Now we look no way about motor function.Perhaps we are standing alone at this stage.Who can guide us?
Hope God will help us
hi
i am very interested in knowing about Jawad Pasha. My uhncle to in in a Minimal con state after lack of oxygen to his brain after a heart attack. Its day 13 and he for the last 5 days he has regained some conscousnes, he looks around for long periods and moves his arms and legs very occasionally...just hoping he will continue to improve every day.
Dear Gurdeep
Hope for early recovery of your uncle.He seemed to be a much better condition than Jawad.Jawad Pasha could not open his eyes or move even a finger for several weeks after accident.Please take care of his health and rehab support is very necessary.Don't leave him alone and if you are in India ,give him Soup(yakhni) of home kept hen(Desi murghi)
hi there..we live in london. it will be a month tomorrow since he had the attack. he is making steady progress..doctors now say he may be above minimal conscous state. he is trying to talk but we cant make out what he is saying, his voice is very low and husky, he also nods yes and no too. he is able to swallow and is moving is legs aroud more..so i am very glad iof the progress..i just hope jawad continues to make progress..keep me posted! regard Gurdip
Thank you Gurdeep.
Hope your brother improving,As far as our experience say these patients need more and more personal care .They need 24 hours attachment.Just put yourself on his place and think of his needs,you will know all.When they open eye in night any time,they need some one taking care of them. It ia a very very slow process and you should be prepare for this. Hope you will see him smiling even laughing very soon. 'Rab Rakha'
Hi Gurdeep.
Hoe is ur uncle now, Jawad Pasha is improving.
There is another new story,
A man thought to have been in a vegetative state for 23 years was conscious throughout the entire ordeal.
Rom HoubenRom Houben of Belgium was diagnosed as being in a vegetative state after a car wreck, but doctors now know the 46-year-old man was aware of his surroundings, heard what was being said, but couldn't respond. He has been provided with equipment to read and type since this discovery, and with therapy, he is now able to communicate. Bobby Schindler of Terri's Foundation reacts to the news.
"This isn't the first time we've heard this or we've read that something like this has happened where someone has emerged from what doctors were saying...was a persistent vegetative state, and I think it illustrates why we need to stop dehydrating to death these people who are labeled in this highly subjective diagnosis," Schindler contends.
Doctors confirm that patients classified as being in a vegetative state are often misdiagnosed, and that "unconsciousness" stamp is one which patients rarely escape. This confirmation leaves one to wonder, says Schindler, if many people who have died in a "vegetative state" were misdiagnosed.
"There's no way of telling," Schindler notes. "But don't take my word for it about the inaccuracy of this PVS diagnosis. All you need to do is to look at some recent research that has been done where they have been finding that the Persistent Vegetative State diagnosis is misdiagnosed upwards of 50 percent of the time."
He says it is especially shocking because this diagnosis was used for euthanasia advocates to obtain the court order that killed his sister, Terri Schindler Schiavo, by removing her feeding and hydration tubes in March 2005.
Why these doctor never contacted me to see Jawad Pasha. He is a more perfact evidence.
The case of Mr. Houben is quite complicated, with his verbal output (through the discredited use of facilitated communication) almost certainly bogus. That's not to say that he is not in a locked-in syndrome (rather than PVS). The best summary is at NeuroLogica blog - Man in Coma 23 Years – Is He Really Conscious?
Thank you very much. I have another case.He is just 17 year old Muhammad Hussain Kakar from a village near Pishin Quetta Pakistan.He injured in a road accident last year. He came in my contact during March this year.There was no medical facility available to him exept a paramedical who changed his nasal feeding tube weekly after being discharged from a hospital at Quetta. He was having bed sores, Cotructures in arms and legs and no gauidance.Also cotinuous Seizures/Fits were reported. A perfect PVS at that time without any responce or movement but a paramedical who has worked with me for my son for three years whom I first sent to see the boy told me that he seems to be responding but no way to do any thing. We used our experience and by grace of God within last seven months he is healthy,Smiling,Sometime laughing on Jokes,Started a little eating by mouth, moving his body a little but without control. Perhaps he is too without motor function like Jawad Pasha but he too seems conscious and aware. His seizure is also much controlled.
I have tried to communicate about him time to time on different sites.
Now your turn to search about these two and write a new blog.
I have tried to write something to help others. You can read that at this link. What to do when your loved one is diagnosed as Persistent Vegetative or Minimally Conscious State ?
Here's the link to Anwer's piece:
http://silencelives.blogspot.com/2009/12/what-to-do-when-your-loved-one-is.html
I have another related news. A therapist Mr Naeem told me that he is working with a patient diagnosed as locked in syndrome after an accident just four months ago. I and Mr Naeem ate in discussion about Jawad Pasha since long . He told me that he is working with an idea to take help from the habits and do it as early as possible because the passage of of the time in bed lost many habits. He says that he is achieving very good results.The patient is improving. Hope we shall do something for the patients in Persistent vegetative ,Minimally conscious state or locked in syndrome.
One day , This was the only site where I find some criticism on the approach of neurologists about Persistent Vegetative State and Minimally Conscious State . Now the world has been changed. I was also trying to tell the world about that due to my personal experience about my son Jawad Pasha and others. We are still much ahead and knew what they only image through scans. We have now understanding about more fast recovery but you see in spite of my hundreds posts nobody bothered to ask even any question yet.
Congratulation for your successful effort.
Thanks, Anwer. Your persistence and care have been inspiring. Here's the latest paper from Owen, Laureys et al.:
Monti MM, Vanhaudenhuyse A, Coleman MR, Boly M, Pickard JD, Tshibanda L, Owen AM, Laureys S. Willful Modulation of Brain Activity in Disorders of Consciousness. N Engl J Med. 2010 Feb 3. [Epub ahead of print].
BACKGROUND: The differential diagnosis of disorders of consciousness is challenging. The rate of misdiagnosis is approximately 40%, and new methods are required to complement bedside testing, particularly if the patient's capacity to show behavioral signs of awareness is diminished. METHODS: At two major referral centers in Cambridge, United Kingdom, and Liege, Belgium, we performed a study involving 54 patients with disorders of consciousness. We used functional magnetic resonance imaging (MRI) to assess each patient's ability to generate willful, neuroanatomically specific, blood-oxygenation-level-dependent responses during two established mental-imagery tasks. A technique was then developed to determine whether such tasks could be used to communicate yes-or-no answers to simple questions. RESULTS: Of the 54 patients enrolled in the study, 5 were able to willfully modulate their brain activity. In three of these patients, additional bedside testing revealed some sign of awareness, but in the other two patients, no voluntary behavior could be detected by means of clinical assessment. One patient was able to use our technique to answer yes or no to questions during functional MRI; however, it remained impossible to establish any form of communication at the bedside. CONCLUSIONS: These results show that a small proportion of patients in a vegetative or minimally conscious state have brain activation reflecting some awareness and cognition. Careful clinical examination will result in reclassification of the state of consciousness in some of these patients. This technique may be useful in establishing basic communication with patients who appear to be unresponsive. Copyright 2010 Massachusetts Medical Society.
I have to share a further recovery. Jawad Pasha is still without motor function but now a days he is using his muscles to share . Especially when I myself starts his late night small session of exercise and ask him to move himself , He tries. I am not good in English so I can not narrate clearly but I feel very clearly his movement. I am hopeful that if it continued,in next few months he will be able to sit or stand with a very little help.
I have told you some months ago about one Muhammad Hussain. You will be happy to know that he has started talking by repeating the words .His feeding tube has been removed and he is now taking food by mouth. God is great. This all happen without any therapist or medical support. Actually nothing was is available to them. Now that family is too working on another such patient. 11 years old Azizullah of a remote villahe Kali Usman of same area, We hope for more quick results.
I have told you earlier about one Muhammad Hussain of Pishin, Quetta, Pakistan. By grace of god he is now talking by repeating words and his feeding tube has been removed. Now taking food by mouth.
Thank you all for sharing your stories, it's very hard for relatives of patient and I hope you see daily improvement in your beloved patient.
I am curious to know how is Javad Paaha doing now? My brother 42y also is in minimally C.state, little movement but started to smile and laugh at jokes after a year of his TBI. God is great, thank you.
Post a Comment
<< Home